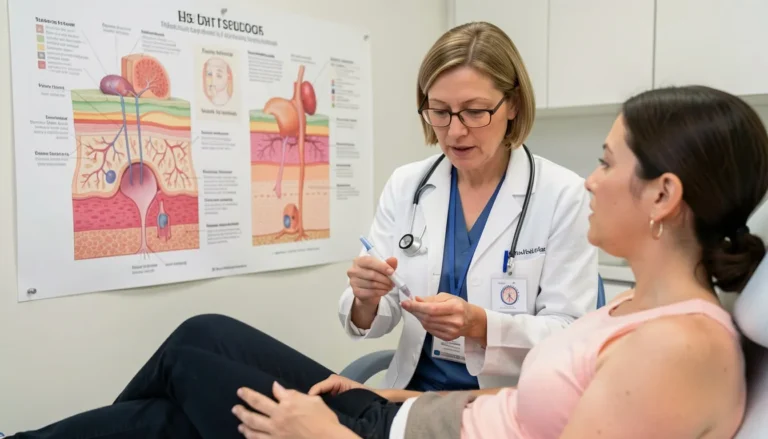
Cortisol Skin: How Stress Hormones Cause Breakouts and How to Fix It (2026 Guide)
Cortisol Skin: The Comprehensive 2026 Guide to Stress-Induced Dermatitis, Neuro-Cosmetics, and the Brain-Skin Axis

In the fast-paced landscape of 2026, the American skincare consumer has moved beyond “miracle creams” and surface-level aesthetics. We have entered the era of Psychodermatology. As mental health and physical appearance become inextricably linked, a new clinical term has dominated dermatological journals: Cortisol Skin.
If you have ever experienced a sudden, painful breakout before a wedding, or noticed your skin looking “gray” and depleted after a month of overtime at work, you have witnessed the power of the Brain-Skin Axis. This guide serves as the definitive resource for understanding how the “stress hormone” dictates your complexion and how you can reclaim your glow through science-backed interventions.
The Science of Psychodermatology: Defining Cortisol Skin
To understand Cortisol Skin, we must first define the hormone at its center. Cortisol is a glucocorticoid, a steroid hormone produced by the adrenal glands sitting atop your kidneys. In the natural world, it serves as our “Survival Signal,” a biological catalyst designed to provide a burst of glucose, energy, and heightened focus during life-threatening “fight or flight” situations.
However, in 2026, the modern American lifestyle has hijacked this primitive survival mechanism. Our “threats” are no longer apex predators; they are endless email chains, gridlock traffic, and the unrelenting blue light of digital overstimulation. When this survival switch stays “on,” the body enters a state of chronic hyper-cortisolemia. This systemic overflow doesn’t just affect your heart rate or sleep—it manifests visibly as Cortisol Skin.
The Embryonic Connection: The Ectoderm Secret
The reason your skin reacts so violently to your thoughts lies in the very first weeks of your existence. During the earliest stages of human embryology, the brain and the skin are formed from the exact same layer of cells, known as the ectoderm.
This shared biological ancestry means that the central nervous system and the integumentary system (your skin) remain “hard-wired” together for life. This link is now formally recognized by dermatologists as the Brain-Skin Axis. When your brain perceives a psychological threat, that stress doesn’t stay confined to your mind—it travels instantly through a complex network of neuropeptides and nerve endings directly to your skin cells. This immediate, bidirectional chemical communication is the fundamental cause of Cortisol Skin.
The Rise of Psychodermatology in 2026
The emergence of Psychodermatology as a mainstream clinical field in the USA highlights a major shift in how we view beauty. The “topical-only” mentality is being abandoned. Scientists have discovered that skin cells, specifically keratinocytes and sebocytes, actually have their own local receptors for stress hormones.
This means your skin isn’t just a passive victim of the brain’s stress; it can actually produce its own “local” cortisol in response to environmental triggers. This localized production creates a feedback loop that traps the complexion in a state of perpetual irritation. When we talk about Cortisol Skin, we aren’t just talking about a few “stress spots”; we are talking about a systemic failure of the skin’s ability to protect, repair, and renew itself.
The 2026 Digital Stress Epidemic
A new factor contributing to Cortisol Skin in 2026 is “Digital Stress.” Clinical studies now show that the high-frequency blue light from our devices combined with the “doomscrolling” dopamine-cortisol cycle creates a unique type of dermal fatigue. This “Screen-Induced Cortisol Skin” is characterized by a specific type of dullness and infraorbital (under-eye) inflammation that traditional skincare routines fail to resolve because they ignore the neurological root.
Key Takeaways for Section 1:
The Ectoderm: The brain and skin are biological siblings.
The Brain-Skin Axis: The highway that transports stress signals to your pores.
Local Production: Your skin can produce its own cortisol, making Cortisol Skin a self-sustaining cycle if not treated at the source.
The Biological Mechanism: How Stress Rewires Your Dermis
When the body enters a chronic state of “fight or flight,” cortisol doesn’t just circulate—it invades. In the clinical world of 2026, we describe this as Dermal Dysregulation. Here is a layer-by-layer breakdown of how Cortisol Skin manifests across your integumentary system:
The Stratum Corneum (The Epidermal Barrier): Lipid Dissolution
The outermost layer of your skin, the stratum corneum, relies on a “brick-and-mortar” structure composed of ceramides, cholesterol, and free fatty acids. High systemic levels of cortisol act as a biological solvent, effectively dissolving these essential lipids.

This process leads to a catastrophic rise in Transepidermal Water Loss (TEWL). When the barrier is compromised by Cortisol Skin, moisture evaporates into the air while external irritants (pollution, bacteria, allergens) seep into the deeper layers. This explains the paradoxical “Oily-Dry” sensation: Cortisol Skin often feels greasy on the surface due to compensatory oil production, yet feels painfully tight, flaky, and dehydrated underneath.
The Dermis: Collagen Fragmentation and “Inflamm-aging”
In 2026, the most researched topic in Psychodermatology is “Inflamm-aging”—the accelerated aging of cells due to chronic stress. Within the dermal layer, cortisol acts as a primary inhibitor of fibroblast activity. Fibroblasts are the “factory cells” responsible for producing Hyaluronic Acid, Collagen, and Elastin.
When Cortisol Skin becomes a chronic state:
Hyaluronic Acid Depletion: The skin loses its internal “sponge,” leading to a hollowed, sunken appearance.
Collagenase Activation: Cortisol triggers a destructive enzyme called MMP-1 (Collagenase). This enzyme physically “chops” through existing collagen fibers like microscopic scissors.
Glycation: Stress-induced glucose spikes can lead to glycation, where sugar molecules attach to proteins, making collagen stiff and brittle. The result? The premature appearance of deep-set “stress lines” and a noticeable loss of facial “bounce.”
The Pilosebaceous Unit: The Androgen-Sebum Spike
Cortisol rarely travels alone; it is almost always accompanied by a surge in adrenal androgens (like DHEA-S). These hormones serve as a direct “on switch” for your sebaceous glands.
However, the oil produced in Cortisol Skin is biologically different from standard teenage sebum. It is hyper-viscous—meaning it is thicker and stickier. This “sticky sebum” combines with the dead skin cells that aren’t shedding properly due to slowed turnover. The result is a high frequency of Cystic Acne. Because the inflammation is so deep, these blemishes often feel “trapped” beneath the surface, causing significant pain and pressure without ever reaching a head.
The Vascular System: Micro-Circulatory Stasis
A lesser-known biological effect of Cortisol Skin is its impact on blood flow. Cortisol causes vasoconstriction—the narrowing of the blood vessels. When you are stressed, your body redirects blood flow to your heart and muscles (the “survival” organs) and away from your skin.
Without adequate blood flow, the skin is deprived of oxygen and essential nutrients. This is why Cortisol Skin is often characterized by a “sallow” or grayish undertone. Furthermore, this lack of circulation slows down the removal of metabolic waste, which contributes to the under-eye puffiness and “toxic” appearance common during high-cortisol periods.
The Neuro-Sensory Response: Hyper-Reactivity
Finally, Cortisol Skin involves the sensitization of the skin’s nerve endings. Cortisol increases the production of Substance P, a neuropeptide that transmits pain and itching signals. This explains why people with Cortisol Skin often report that their face “hurts” or feels “tingly” and “hot,” even when no visible rash is present. Your skin’s nervous system is essentially on high alert, making it react aggressively to even the most “clean” or “gentle” skincare ingredients.
Identifying the Symptoms: Is it Regular Acne or Cortisol Skin?
Distinguishing Cortisol Skin from standard hormonal fluctuations is the most critical step in choosing an effective treatment protocol. While puberty-driven acne is primarily a byproduct of excess sebum and bacteria, and adult hormonal acne is dictated by the 28-day menstrual cycle, Cortisol Skin is defined by Hormonal Reactivity.
Unlike cyclical acne, Cortisol Skin does not wait for a specific time of the month. It strikes in direct correlation with your nervous system’s “allostatic load”—the cumulative wear and tear on the body. Here are the clinical markers used by 2026 psychodermatologists to identify the condition.
The “U-Zone” Signature: Mapping Stress Breakouts
While traditional acne often dominates the oily T-zone (forehead, nose, and upper chin), Cortisol Skin breakouts have a very specific geographic preference: the U-zone.
This includes the jawline, the lower chin, and the sides of the neck.Because cortisol triggers an inflammatory cascade in the deeper dermal layers, these blemishes are rarely superficial whiteheads. Instead, Cortisol Skin presents as deep, tender nodules. These are often “blind pimples” that feel like hard knots under the skin. They are significantly redder and more painful than standard acne because the cortisol has sensitized the local nerve endings, making every touch feel magnified.
Textural Dehydration and “Sallow” Tone: The Loss of Vitality
One of the most overlooked symptoms of Cortisol Skin is the sudden loss of “translucency.” In a healthy state, your skin reflects light due to high water content and smooth cellular turnover. However, because stress restricts microcirculation, blood flow is redirected away from the face to the core muscles.
This results in a grayish, sallow, or “tired” appearance. Furthermore, Cortisol Skin suffers from Textural Dehydration. This is a specific state where the skin’s surface looks “crepey” or finely lined (like crumpled tissue paper) despite being oily to the touch. This “Oily-Dry” paradox is a definitive clinical sign that cortisol has dissolved your protective lipid barrier.
The Chronic Flush: Neuro-Sensitivity and Stress-Induced Rosacea
In 2026, we have seen a massive rise in “Neuro-Sensitivity,” often misdiagnosed as standard Rosacea. High cortisol levels increase the skin’s production of neuropeptides, which are chemicals that talk to your nerves. This leads to a hyper-reactive state where the skin’s “alarm system” is always on.
For someone with Cortisol Skin, this manifests as:
The Sudden Flush: Your face turns bright red during a stressful conversation or a frantic morning.
The “Burning” Sensation: Skincare products that were once your “holy grail” suddenly cause a stinging or itching sensation.
Persistent Erythema: A lingering redness in the center of the face that doesn’t subside even after you’ve cooled down physically.
Periorbital Fatigue: The Stress-Eye Connection
The skin around the eyes is the thinnest on the human body, making it a primary “canary in the coal mine” for Cortisol Skin. Chronic cortisol elevation causes the body to retain salt and water in the infraorbital tissues, leading to persistent under-eye puffiness.
Additionally, because cortisol impairs blood vessel health, you may notice “Vascular Dark Circles”—a blue or purple tint under the eyes caused by stagnant, deoxygenated blood. This is often the first visible symptom of Cortisol Skin and serves as a warning that your internal stress levels are reaching a breaking point.
Delayed Re-Epithelialization (Slow Healing)
If you notice that a small blemish or a tiny scratch now takes two weeks to heal instead of three days, you are likely dealing with Cortisol Skin. Cortisol inhibits the migration of new skin cells to the surface. This “stalled” healing process not only keeps inflammation active for longer but also increases the likelihood of Post-Inflammatory Hyperpigmentation (PIH)—those stubborn dark spots that remain long after the breakout is gone.
The 2026 Ingredient Spotlight: The Rise of Neuro-Cosmetics
Traditional skincare has long been obsessed with “correction”—using aggressive acids to exfoliate or heavy oils to hydrate. However, Cortisol Skin is not a surface issue; it is a neurological one. In 2026, the industry has pivoted toward Neuro-Cosmetics: bio-active ingredients designed to modulate the skin’s sensory receptors and downregulate the inflammatory “noise” coming from the brain.
To heal Cortisol Skin, we must use ingredients that don’t just treat the symptom, but actually intercept the stress signal at the cellular level.
Topical Adaptogens: The “Biological Thermostats”
Adaptogens like Ashwagandha, Rhodiola Rosea, and Holy Basil (Tulsi) have made a definitive jump from wellness teas into high-potency clinical serums. These botanicals work by stabilizing the HPA-like axis within the skin itself.
When Cortisol Skin is triggered, your keratinocytes (skin cells) actually produce their own local cortisol. Topical adaptogens act as competitive inhibitors; they sit on the cortisol receptors, effectively “locking” them so the stress hormone cannot deliver its inflammatory message. This prevents the cascade of redness and collagen breakdown before it even begins. In 2026, Rhodiola, in particular, is prized for its ability to boost beta-endorphins in the skin, providing a “hormetic” effect that makes the skin more resilient to future stress.
Ectoin: The “Extremolyte” Molecular Shield
If 2024 was the year of Hyaluronic Acid, 2026 is the year of Ectoin. Originally discovered in halophilic (salt-loving) bacteria that thrive in the world’s harshest deserts and salt lakes, Ectoin is a powerful Extremolyte.
In the context of Cortisol Skin, Ectoin works through a process called “preferential hydration.” It forms a million-molecule-thick “hydro-shell” around skin cells and proteins. This shell acts as a physical buffer. When stress hormones attempt to trigger lipid dissolution (the thinning of your skin barrier), Ectoin keeps the cellular structure stable. It is essentially an “anti-stress” armor that prevents the dehydration and DNA damage that typically characterizes a high-cortisol complexion.
Expert Recommended: Combat Cortisol Skin with our Top-Rated Ectoin Repair Serum
Microencapsulated Magnesium: The Transdermal Relaxant
Magnesium has long been known as the “master mineral” for internal relaxation, but 2026 technology has finally perfected its delivery to the dermis. Standard magnesium salts are often too large to penetrate the skin barrier effectively. However, Microencapsulated Magnesium uses lipid-spheres to carry the mineral into the deeper layers where Cortisol Skin damage occurs.
Magnesium works by inhibiting Substance P, the neuropeptide responsible for the “burning” and “stinging” sensations associated with neuro-sensitivity. By stabilizing the cellular repair mechanism, it helps “turn off” the hyper-reactive state of the skin. It also aids in ATP production, giving cells the energy they need to repair the collagen fragmentation caused by chronic stress.
Palmitoyl Tripeptide-8: The “Neuro-Soother”
A new addition to the 2026 neuro-cosmetic arsenal is Palmitoyl Tripeptide-8. This is a multi-functional neuropeptide designed specifically to prevent and soothe neurogenic inflammation. In clinical trials for Cortisol Skin, this peptide has shown a remarkable ability to reduce the dilation of blood vessels (the “flush”) and lower the threshold of skin sensitivity. It works by mimicking the body’s natural anti-inflammatory signals, essentially “telling” the skin to ignore the brain’s stress commands.
The Role of Pre- and Post-Biotics
Finally, we cannot discuss Cortisol Skin without the microbiome. Stress drastically alters the pH of the skin, killing off “good” bacteria and allowing C. acnes and Staph to flourish. 2026 formulations for stress-induced skin now include Lactobacillus Ferment and Inulin to re-acidify the skin mantle. By restoring the microbiome, these ingredients ensure that even when cortisol levels are high, the skin’s first line of defense remains intact.
The “Stress-Shield” Routine: A Clinical Protocol
If you are currently experiencing Cortisol Skin, your goal is to “De-escalate.” Aggressive acids (like high-percentage Glycolic or Salicylic acid) will only worsen a stress-damaged barrier.
The Morning: Resilience and Protection
Non-Stripping Cleanser: Use a milk or oil-based wash to preserve the delicate lipid barrier.
Vitamin C + Ferulic Acid: This duo neutralizes the oxidative stress that cortisol produces.
Mineral SPF: Zinc Oxide is naturally anti-inflammatory, making it the perfect choice for the sensitive nature of Cortisol Skin.
The Evening: Deep Barrier Repair
Double Cleanse: Use a balm to melt away pollutants, followed by a hydrating cleanser.
Niacinamide (5%) Serum: Niacinamide is the “architect” of the skin barrier, helping to rebuild the lipids that cortisol dissolves.
Ceramide-Rich Moisturizer: Look for a “3:1:1” ratio of ceramides, cholesterol, and fatty acids to seal the skin.
Beyond the Bottle: Managing the Brain-Skin Axis
In 2026, we recognize that you cannot “cream” your way out of a high-cortisol lifestyle. To truly heal Cortisol Skin, you must address the nervous system.
Vagus Nerve Stimulation
The Vagus nerve is the “off-switch” for the body’s stress response. Simple techniques like “The 30-Second Cold Splash” or deep diaphragmatic breathing can instantly lower systemic cortisol. When your heart rate drops, the inflammatory signals to your skin stop, providing an immediate “calming” effect on Cortisol Skin redness.
The Digital Sunset and Melatonin
Digital stress is a primary driver of Cortisol Skin in the USA. Blue light doesn’t just damage the eyes; it suppresses Melatonin, the body’s most powerful repair hormone. By implementing a “Digital Sunset” (no screens 60 minutes before bed), you allow Melatonin to rise, signaling your skin to begin its nightly repair of Cortisol Skin damage.
The 3-Minute Facial Massage
Physical touch releases Oxytocin, the biological antagonist to cortisol. A gentle nightly massage—using light, upward strokes—can physically lower the stress hormones in the facial tissue, promoting lymphatic drainage and restoring the glow that Cortisol Skin steals.
Frequently Asked Questions (FAQs): Managing Cortisol Skin
Q: Can I use Retinol or Tretinoin if I am currently experiencing Cortisol Skin?
A: You should proceed with extreme caution. During an active Cortisol Skin flare, your lipid barrier is physically compromised (thinned out). Introducing a potent retinoid can lead to “Retinoid Dermatitis”—an aggressive inflammatory response that mimics a chemical burn. In 2026, the clinical recommendation is to “Pause and Prime.” Switch to Bakuchiol, a plant-based terpenoid that provides similar collagen-boosting benefits without the irritation, until your moisture barrier is fully restored.
Q1: How exactly does diet influence the severity of Cortisol Skin?
A: The relationship is driven by the Insulin-Cortisol Loop. High-glycemic foods (refined sugars, white bread, processed snacks) cause a rapid spike in blood glucose. This triggers an insulin surge, which subsequently stimulates the adrenal glands to release more cortisol. To heal Cortisol Skin from within, prioritize:
Omega-3 Fatty Acids: Found in walnuts and salmon, these reduce systemic inflammation.
Probiotic Foods: Kimchi or Kefir help stabilize the gut-skin axis.
Low-GI Complex Carbs: Steel-cut oats and quinoa keep blood sugar stable, preventing the hormonal spikes that feed Cortisol Skin.
Q2: Is Cortisol Skin a permanent condition?
A: Fortunately, no. Unlike genetic skin types (like true oily or dry skin), Cortisol Skin is a reactive physiological state. Once you identify your stress triggers, stabilize your HPA-axis (through lifestyle), and repair the epidermal barrier with neuro-cosmetic ingredients like Ectoin and Ceramides, your skin can return to its natural, radiant state. It has to do with biology, not fate.
Q3: Will a standard “Acne Face Wash” help clear Cortisol Skin breakouts?
A: Paradoxically, most standard acne washes can make Cortisol Skin worse. While a salicylic wash might be effective for localized acne around the nose, using it on a stress-damaged barrier strips away remaining lipids, leading to more inflammation. For Cortisol Skin, you need a “non-stripping” pH-balanced cleanser that removes debris without disrupting the acid mantle.
Q4: Can supplements like Ashwagandha help heal Cortisol Skin?
A: Yes, ingestible adaptogens can lower systemic cortisol levels, which reduces the “fuel” for Cortisol Skin. However, for targeted results, 2026 research suggests a “dual-action” approach: taking a high-quality Ashwagandha supplement internally while applying a topical adaptogen serum to treat the local skin receptors.
Conclusion: Healing Cortisol Skin from Within
As we have explored in this 2026 guide, the secret to a resilient, glowing complexion is no longer found in a single “miracle” ingredient. Instead, it lies in the delicate balance of the Brain-Skin Axis. Cortisol Skin is not an enemy to be fought with harsh chemicals; it is a sophisticated biological signal from your body. It is your skin’s way of communicating that your internal pace is exceeding your biological capacity to recover.
By adopting a Psychodermatology mindset—combining high-performance neuro-cosmetics like Ectoin and Magnesium with nervous system regulation—you can move beyond simply treating symptoms. You can build a complexion that is not only clear but stress-resilient. In an age of digital overstimulation and high-pressure lifestyles, the ultimate luxury is a calm mind and a calm barrier.
Medical Disclaimer
Here, “Cortisol Skin” refers to the skin conditions caused by high levels of stress hormones.This information is for educational purposes and is not intended to replace professional medical advice, diagnosis, or treatment. Always seek the advice of a board-certified dermatologist or other qualified health provider with any questions you may have regarding a medical condition or skin disorder.