Recurrent Groin Abscess ICD-10 Code: Diagnosis, Chronic Care, and 2026 Treatment Guide
Understanding Chronic Groin Abscesses: A Modern Clinical Approach
Introduction: Why Do Groin Abscesses Keep Coming Back?
For many, a groin abscess is seen as a “one-off” annoyance—a simple case of an ingrown hair or a clogged sweat gland that clears up with a quick round of antibiotics. However, for a significant number of individuals, these painful nodules are not isolated incidents but recurring characters in a persistent and debilitating script.
Understanding why these infections return requires looking beyond the surface of the skin and into the underlying biology of why certain areas of the body become “hotspots” for inflammation. When these episodes repeat, clinicians must move beyond general diagnosis and apply the specific Recurrent Groin Abscess ICD-10 Code to trigger advanced care pathways.
The “Chronic Cycle”: Infection vs. Condition
It is vital to distinguish between a transient infection and a recurrent condition:
One-time Infection: Usually caused by external bacteria (like Staphylococcus aureus) entering a break in the skin. Once treated, the tissue heals, and the threat is gone.
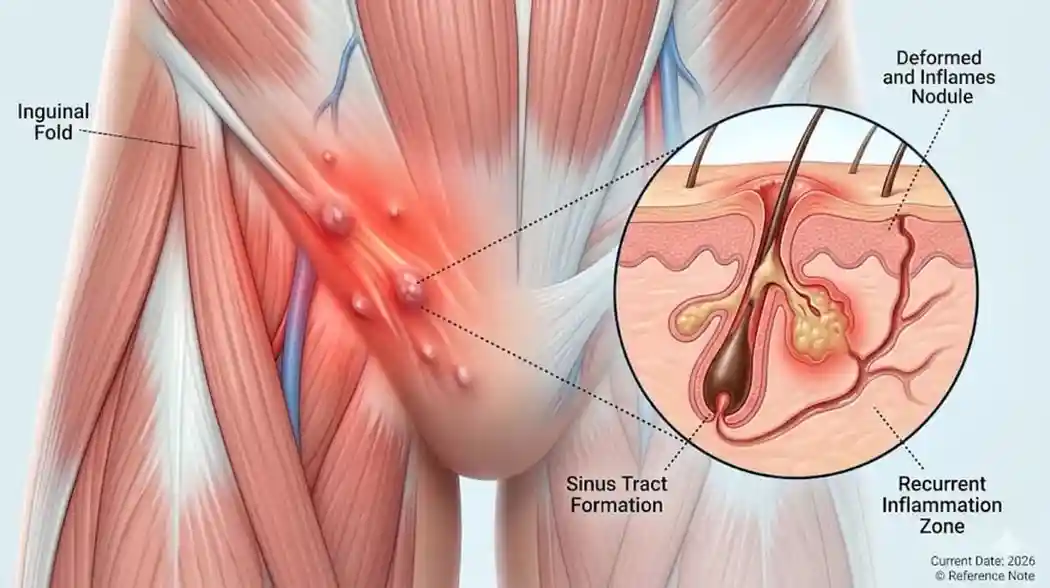
Recurrent Condition: Often indicative of Hidradenitis Suppurativa (HS) or chronic follicular occlusion. Here, the issue isn’t just “germs”; it’s a structural failure of the hair follicle and an overactive local immune response. The “cycle” occurs because the underlying sinus tracts (tunnels under the skin) remain even after the swelling goes down, acting as reservoirs for future flare-ups.
The True Impact: More Than Skin Deep
The burden of chronic groin nodules extends far beyond physical discomfort:
Physical Limitations: Constant inflammation in the inguinal folds can severely restrict mobility, making walking, exercising, or even sitting for long periods agonizing.
Psychological Toll: The “hide and seek” nature of these abscesses often leads to anxiety, body image issues, and social withdrawal. There is a specific kind of mental fatigue that comes with never knowing when the next flare-up will occur.
2026 Guidelines: A Shift in Strategy
The medical landscape has shifted significantly this year. The 2026 Clinical Standards now emphasize that a Recurrent Groin Abscess ICD-10 Code should rarely be treated with “reactive” localized care alone (like repeated lancing).
Instead, the gold standard has moved toward:
Systemic Modulation: Using biologics and JAK inhibitors to “turn down” the body’s inflammatory dial.
Early Surgical De-roofing: Moving away from simple drainage and toward removing the “tunnels” to prevent the abscess from having a place to return.
Hormonal & Metabolic Mapping: Dealing with the underlying causes of follicular collapse, such as insulin resistance or hormonal changes.
Understanding the Recurrent Groin Abscess ICD-10 Code
When a patient sees their primary care physician or a dermatologist, the physical symptoms are translated into a standardized alphanumeric code. For those navigating chronic groin issues, understanding the Recurrent Groin Abscess ICD-10 Code system can help demystify billing statements and ensure that the treatment plan matches the true severity of the condition.
The Diagnostic Toolkit: Common ICD-10 Codes
| ICD-10 Code | Clinical Definition | When It’s Used |
| L02.214 | Cutaneous abscess of the groin | The “primary” code. Used for a standard, acute abscess (boil) that is localized and requires immediate drainage or antibiotics. |
| L73.2 | Hidradenitis Suppurativa (HS) | The “chronic” Recurrent Groin Abscess ICD-10 Code. Used when abscesses are recurrent, bilateral, and show signs of scarring or “tunneling.” |
| L08.89 | Other specified local infections | A “catch-all” used for atypical recurrences that don’t quite fit the criteria for HS but are more complex than a simple bacterial boil. |
| L05.01 | Pilonidal cyst with abscess | Used specifically if the recurrence is near the tailbone or perianal area, which can be mistaken for a standard groin abscess. |
Medical Authority Note: Proper application of the Recurrent Groin Abscess ICD-10 Code is vital for accessing 2026-approved systemic therapies. For instance, many insurance providers require an L73.2 diagnosis before they will approve the use of advanced biologics or specialized surgical “de-roofing” procedures.
Why the Recurrent Groin Abscess ICD-10 Code Matters for the Patient
Specialist Access: An L73.2 code often triggers a faster referral to a specialized “HS Clinic” or a dermatologist rather than a general surgeon.
Insurance Coverage: Chronic codes justify the need for long-term maintenance medications rather than just a one-time antibiotic script.
Medical History Accuracy: It distinguishes an “unfortunate one-time event” from a “chronic systemic condition” in a permanent medical record, ensuring doctors don’t keep repeating ineffective treatments.
Diagnosis: Is it an Infection or a Chronic Condition?
The most common mistake in treating groin issues is addressing a persistent condition as if it were a one-time infection. While they may look identical on the surface, the “behavior” of the lesion and the underlying anatomy tell the true story. Correctly identifying these signs allows your doctor to apply the appropriate Recurrent Groin Abscess ICD-10 Code for long-term care.
1. Infected Follicle vs. Hidradenitis Suppurativa (HS)
Determining the difference often comes down to what is happening beneath the surface of the skin.
Infected Follicle (Folliculitis): Typically appears as a single, painful red bump centered around a hair. It may come to a “head,” drain, and disappear completely within a week.
Hidradenitis Suppurativa (HS): The hallmark of HS is recurrence in the same spot and the presence of sinus tracts (tunnels). These are narrow channels under the skin that connect multiple abscesses. If you feel a firm, rope-like structure beneath the skin even after the abscess has drained, it is likely a chronic condition requiring an L73.2 diagnosis.
2. The “Double-Headed” Comedone
A specific clinical sign that points toward the chronic Recurrent Groin Abscess ICD-10 Code (L73.2) is the “tombstone” or double-headed comedone. These look like two or more blackheads appearing very close together in an area of prior inflammation. They occur because the hair follicle has structurally collapsed, creating a multi-channeled opening to the surface. If you see these in the groin or armpit area, it is a strong indicator of a systemic follicular issue.
3. Diagnostic Tools: The 2026 Standard
In 2026, two specific tools have become the gold standard for validating a Recurrent Groin Abscess ICD-10 Code:
High-Frequency Skin Ultrasound: This allows doctors to see sub-epidermal tunnels and fluid collections that aren’t visible to the naked eye. It is essential for staging the condition before it worsens.
Bacterial Cultures: While most chronic abscesses are inflammatory, cultures rule out secondary infections like MRSA, ensuring any prescribed antibiotics are targeted and effective.
4. When to See a Specialist: The “Red Flags”
While chronic nodules are often managed through routine appointments, certain symptoms require immediate intervention to prevent complications:
Cellulitis: A rapidly spreading “sunburn-like” redness that feels hot and expands away from the abscess.
Systemic Symptoms: Fever, chills, or extreme lethargy, which suggest the infection may be entering the bloodstream.
Non-Healing Wounds: Any abscess that continues to drain or remains an “open hole” for more than three weeks.
Clinical Insight: If you have experienced three or more “boils” in the groin or underarm area within a six-month period, the 2026 guidelines recommend a direct referral to a dermatologist for an HS evaluation. Early use of the Recurrent Groin Abscess ICD-10 Code can prevent permanent scarring and tissue damage.
Treatment Protocols (2026 Clinical Standards)
In 2026, the medical community has moved away from “waiting for a flare” to a proactive, multi-modal strategy. Treatment is now categorized by the speed of relief versus the durability of the results, specifically for cases identified under the Recurrent Groin Abscess ICD-10 Code.
1. Acute Care: The “I&D” Trap
While Incision and Drainage (I&D) remains the gold standard for immediate pressure relief in emergency settings, it frequently serves as a palliative measure rather than a permanent cure for recurrent groin abscesses.”
The issue is that I&D solely deals with the fluid (pus). It does not remove the collapsed follicle or the underlying sinus tract.
The Result: Because the “tunnel” remains, bacteria and debris quickly recolonize the space, leading to a repeat flare-up in the exact same spot within weeks or months.
This 2026 clinical chart helps patients and providers identify the correct Recurrent Groin Abscess ICD-10 Code, moving from acute bacterial boils (L02.214) to chronic Hidradenitis Suppurativa (L73.2).
2. Surgical Innovation: Deroofing
For 2026, Deroofing has become the preferred surgical intervention for recurrent nodules (Hurley Stage I and II).
How it Works: Instead of a simple “poke,” the surgeon removes the “roof” of the abscess and the entire tract. After that, the wound is left open to heal from the bottom up.
The advantage is that the reservoir where diseases lurk is eliminated when the tunnel is physically removed.It maintains more healthy tissue than a full broad excision and has a far lower recurrence rate than I&D.
3. Medical Management: Turning Down the Volume
Modern therapy focuses on reducing the body’s overactive inflammatory response so abscesses stop forming in the first place.
Topical & Wash Solutions
Benzoyl Peroxide (5-10%): Used as a “maintenance wash” to reduce bacterial load on the skin surface without causing antibiotic resistance.
Topical Clindamycin (1%): Often applied twice daily to active spots to dampen localized inflammation.
The “Triple Therapy” Antibiotic Approach
When topicals fail, 2026 guidelines suggest a powerful systemic “reset” using a 10–12 week course of three combined antibiotics:
Rifampin
Clindamycin
Metronidazole
Note: This combination is used more for its anti-inflammatory properties than its ability to kill bacteria. It is designed to “cool down” the tissue before surgery or long-term biologic use.
Biologics: The Stage III Standard
For severe, non-healing recurrence (Hurley Stage III), systemic biologics are the frontline defense. These “smart” drugs target specific proteins in the immune system that are overactive in patients coded with the Recurrent Groin Abscess ICD-10 Code (L73.2).
Adalimumab (Humira): The long-standing gold standard for blocking TNF-alpha.
Secukinumab (Cosentyx): A newer 2026 favorite targeting IL-17A. It is particularly effective for patients who did not respond to Adalimumab, significantly reducing the number of “draining tunnels.”
Bimekizumab: Newly expanded in 2026 protocols for its dual inhibition of IL-17A and IL-17F, offering the highest rates of skin clearance seen to date.
Natural Home Remedies & Prevention
Medical treatments provide the foundation, but your daily habits determine the “baseline” of your skin’s health. By managing friction, moisture, and internal inflammation, you can significantly extend the time between flare-ups and reduce the need for acute care under a Recurrent Groin Abscess ICD-10 Code.
1.The“Chemical Shiel“: Antiseptic Washes
The goal of a wash in 2026 isn’t just to be “clean”—it’s to reduce the bacterial load that triggers an overactive immune response.
4% Chlorhexidine (Hibiclens): This is the gold standard for groin folds. Unlike regular soap, it binds to the skin and continues killing bacteria for hours.
Pro-Tip: Do not scrub. Apply it gently to the area, let it sit for 30–60 seconds to activate, and then rinse. Use it 2–3 times a week for maintenance, or daily during an active flare.
Top Expert Choice for Recurrent Abscesses
Dermatologists specify 4% Chlorhexidine (Hibiclens) to break the cycle of infection and deep-clean pores.
Medical Authority Note: Proper hygiene can reduce symptoms of Hidradenitis Suppurativa.
2. Effective Fluid Release: The Epsom Salt and Warm Compress Method.
Never “pop” a groin abscess; the pressure can force infection deeper into the sinus tracts, causing a small bump to become a large, tunneled network.
Epsom Salt Soaks: Magnesium sulfate helps “draw out” fluid by osmotic pressure. A warm (not hot) sitz bath or a saturated compress for 10–15 minutes helps the skin soften, allowing the abscess to drain naturally through the follicle.
2026 Insight: If an abscess is already draining, switch to a “dry” warm compress to avoid macerating (over-softening) the surrounding healthy skin.
3. Anti-Inflammatory Support: Turmeric & Zinc
2026 clinical reviews have solidified the role of specific supplements as “adjunct” therapies for those managed with a Recurrent Groin Abscess ICD-10 Code:
Zinc Gluconate (approx. 90mg/day): Studies show high-dose zinc can significantly reduce the number of inflammatory nodules by stabilizing the follicular lining. Note: Long-term zinc use requires a small copper supplement to prevent deficiency.
Turmeric (Curcumin): Known for its ability to inhibit TNF-alpha (the same protein targeted by expensive biologics), turmeric helps “cool” the systemic inflammation that fuels recurrence.
4. Lifestyle Shifts: The “Environment of the Inguinal Fold”
Recurrence is often a result of Mechanical Stress—the constant rubbing of skin on skin or fabric on skin.
Weight Management: In the 2026 guidelines, weight loss is treated as a clinical intervention. Even a 5-10% reduction in body weight can decrease the “friction coefficient” in the groin folds, leading to fewer ruptured follicles.
The Underwear Audit: Throw away tight, elasticized, or synthetic “moisture-trapping” underwear.
The Fabric: Switch to Bamboo or Micromodal. These fibers are naturally antimicrobial, incredibly smooth (reducing friction), and wick moisture away 4x better than cotton.
The Cut: Opt for seamless “boxer-brief” styles or “boy-shorts” for women. This moves the seams away from the inguinal fold (the crease where the leg meets the body), where most abscesses form.
.Visualizing why standard incision and drainage often fails for the Recurrent Groin Abscess ICD-10 Code (L73.2). Deroofing permanently removes the underlying sinus tracts to prevent recurrence.
FAQs: Common Concerns in 2026
Q1. Can a groin abscess be caused by shaving
Yes, but with a important caveat. Shaving can cause Folliculitis Barbae—a condition where hair is cut so short it curls back into the skin, causing a minor, acute abscess.
However, if you have stopped shaving and the nodules still return in the same spot, the issue is likely structural (like HS) rather than a simple grooming mishap. In 2026, laser hair removal is often recommended as a preventative treatment because it permanently reduces the follicular friction that triggers recurrence.
Q2. Is it contagious
No. One of the biggest psychological burdens of chronic groin abscesses is the fear of passing it to a partner. Whether it is a chronic cyst or Hidradenitis Suppurativa (L73.2), these are not sexually transmitted infections (STIs) and are not transmissible through skin contact. These are issues of internal follicular collapse and immune over-activation—not a surface-level contagion.
Q3. Does diet affect recurrence
The 2026 research is clearer than ever: What you eat can fuel the inflammatory fire.
High-Glycemic Foods: Sugary snacks and white breads spike insulin, which in turn spikes androgens—hormones that increase oil production and “clog” the pores in the groin area.
Dairy: Many patients find that the hormones naturally present in dairy products act as a trigger for new inflammatory nodules.
The “Brewer’s Yeast” Link: Emerging 2026 data suggests that some individuals with the Recurrent Groin Abscess ICD-10 Code (L73.2) have a sensitivity to brewer’s yeast (found in beer and bread). Eliminating it can significantly reduce the frequency of flare-ups.
Conclusion: Managing the Journey
The single most important takeaway for anyone dealing with recurrent groin abscesses is this: Recurrence is a signal, not a failure. If an abscess returns, it is your body’s way of saying that the underlying “infrastructure”—the sinus tracts and follicular units—needs more than just a one-time antibiotic or a quick lancing. Treating the “Chronic Cycle” requires a long-term management plan that combines the right surgical interventions, like deroofing, with systemic immune support.
The Power of the Correct Code
Never underestimate the importance of your medical record. Ensuring your doctor explores the Recurrent Groin Abscess ICD-10 Code (L73.2) early on is the key to unlocking the 2026 standard of care.
An early, accurate diagnosis doesn’t just treat the pain today—it prevents the permanent scarring and mobility issues of tomorrow. By shifting the diagnosis from a simple infection to a chronic condition, you gain access to the specialized biologics and targeted surgeries that were previously out of reach.
You don’t have to live in a cycle of “waiting for the next one.” With the right 2026 protocols, management is not only possible—it is the new standard.
Medical Disclaimer
The information provided in this guide is for educational and informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment.
Consult a Professional: Always seek the advice of your physician, dermatologist, or other qualified health provider with any questions you may have regarding a medical condition or the use of specific ICD-10 codes for billing.
Emergency Symptoms: If you experience signs of a systemic infection—such as high fever, chills, rapidly spreading redness, or extreme pain—seek emergency medical care immediately.
2026 Guidelines: Medical standards and pharmaceutical protocols (such as the use of biologics or “Triple Therapy”) are subject to change. Treatment should only be initiated under the direct supervision of a licensed healthcare professional.
No Doctor-Patient Relationship: Use of this information does not create a doctor-patient relationship. Never disregard professional medical advice or delay seeking it because of something you have read in this guide.