Stop Scarring: 5 Essential Folliculitis Decalvans Treatment Breakthroughs
Comprehensive Guide to Managing Scarring Alopecia and Scalp Recovery
Introduction – The Severity of Folliculitis Decalvans
Folliculitis Decalvans (FD) is a rare and chronic form of primary neutrophilic scarring alopecia. Unlike common hair loss conditions where the follicle remains dormant, FD is characterized by a persistent and aggressive inflammatory process that targets the hair follicle’s permanent structures. To prevent total hair loss, understanding the necessity of early Folliculitis Decalvans treatment is essential for any patient or clinician.
The Clinical Stakes: Why It’s a Medical Emergency
In the world of trichology and dermatology, FD is often viewed with urgency because of the nature of the damage it inflicts:
Permanent Destruction vs. Temporary Shedding: While conditions like Telogen Effluvium involve temporary shedding where the follicle can recover, FD causes cicatricial (scarring) alopecia.
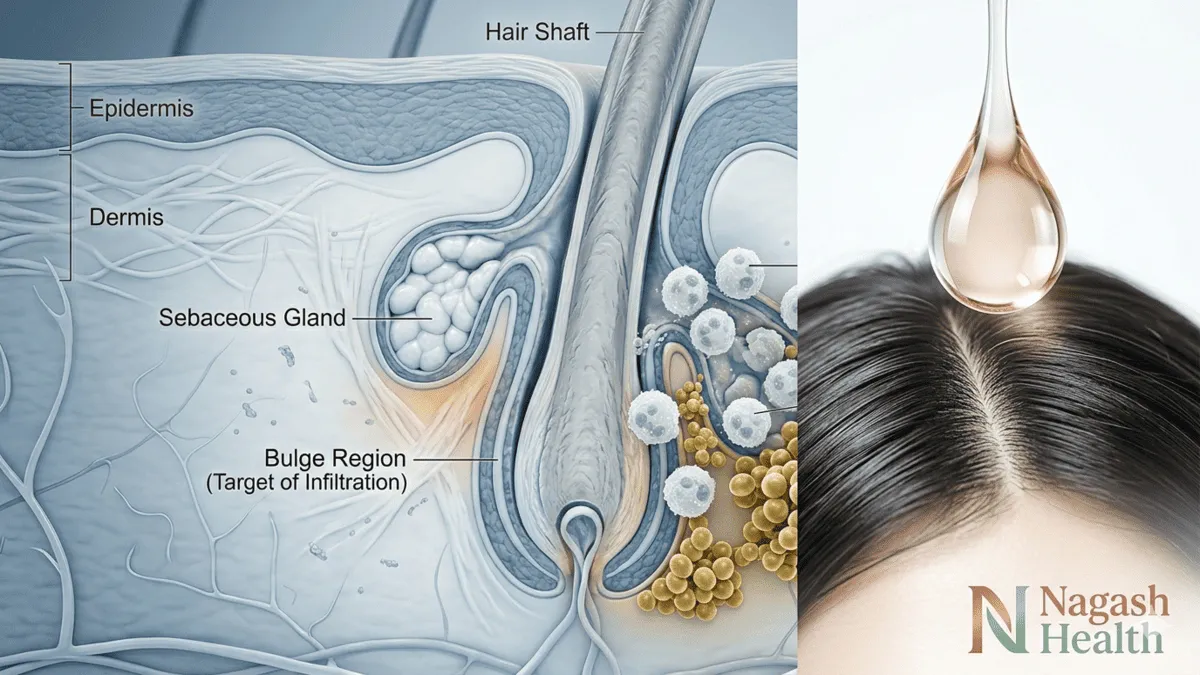
Irreversible Loss: The inflammation destroys the hair follicle’s stem cells in the “bulge” area. Once these cells are destroyed, the follicle is replaced by fibrous scar tissue, making future hair regrowth biologically impossible.
Aggressive Progression: Without rapid clinical intervention, the inflammatory lesions can spread across the scalp, leading to expanding patches of permanent baldness.
ICD-10 Diagnosis for Clinical Reference
For accurate medical documentation, insurance billing in the USA, and clinical tracking, Folliculitis Decalvans is classified under the following diagnostic code:
ICD-10 Code: L66.2 (Folliculitis decalvans)
Recognizing this code is essential for researchers and clinicians to differentiate it from other scarring disorders like Lichen Planopilaris or Frontal Fibrosing Alopecia. Early diagnosis and the immediate initiation of modern Folliculitis Decalvans treatment protocols are the only ways to “arrest” the condition before it reaches the end-state of total follicular obliteration.
Pathophysiology – What Happens Beneath the Scalp?
Understanding the biological mechanisms of Folliculitis Decalvans is crucial for clinical management. It is not merely a surface infection but a complex interplay between external pathogens and an overactive internal immune response. A key component of modern Folliculitis Decalvans treatment involves breaking the biological cycle that leads to permanent scarring.
The Role of Staphylococcus aureus: The “Vicious Cycle”
The primary driver of FD is believed to be a persistent colonization by Staphylococcus aureus. However, unlike a standard infection that clears with basic antibiotics, FD creates a self-sustaining “vicious cycle”:
Bacterial Colonization: S. aureus invades the hair follicle, often protected within a biofilm that makes it resistant to standard immune clearance.
Abnormal Host Response: In predisposed individuals, the immune system views these bacteria as a “superantigen.”
The Cycle: The bacteria trigger an immune response; the immune response causes tissue damage; the damaged tissue then provides an even better environment for more bacteria to thrive, continuing the destruction.
Neutrophilic Inflammation: The Destruction of Stem Cells
The “primary” nature of this alopecia comes from Neutrophils—a type of white blood cell designed to kill bacteria. In FD, these cells become overly aggressive:
Targeting the Hair Bulge: The inflammation specifically targets the bulge region of the hair follicle, which houses vital epithelial stem cells.
Inadvertent Destruction: As neutrophils release toxic enzymes to kill the S. aureus, they inadvertently destroy these stem cells.
Fibrosis: Once the stem cells are gone, the body cannot regenerate a new hair follicle. Instead, the area is repaired with collagen, leading to follicular fibrosis (permanent scarring).
Tufted Folliculitis: The “Doll’s Hair” Hallmark
One of the most distinctive clinical signs discovered during Folliculitis Decalvans treatment consultations is Tufted Folliculitis. This occurs during the chronic phase of the disease:
Multiple Hairs, One Orifice: As the skin between follicles scars and contracts, several previously independent hair follicles are squeezed together.
The “Doll’s Hair” Appearance: This results in “tufts” of 5 to 20 hairs emerging from a single, dilated follicular opening, mimicking the way hair is plugged into a plastic doll’s head.
Clinical Significance: Seeing these tufts is a major diagnostic indicator that the disease has progressed into a scarring phase, requiring immediate aggressive intervention to save the remaining unaffected follicles.
Signs and Symptoms (The Clinical Presentation)
Identifying the early markers of this condition is the first step toward a successful Folliculitis Decalvans treatment plan. Because this disease is progressive, recognizing the transition from simple irritation to active scarring is vital for biological recovery.
Early Warning Signs: The “Pre-Scarring” Phase
Before permanent hair loss occurs, patients often report localized sensations that signal the onset of neutrophilic infiltration:
Scalp Dysesthesia: Patients frequently experience “scalp pain” or a burning sensation, often described as a deep, throbbing ache.
Pruritus (Itching): Intense itching that does not respond to standard over-the-counter anti-dandruff shampoos.
Scalp Tightness: A feeling of tension in specific areas of the vertex (crown), where the inflammation is typically most active.
Active Progression: Clinical Lesions
As the need for clinical Folliculitis Decalvans treatment becomes urgent, the physical symptoms become more visible and severe:
Follicular Pustules: Small, pus-filled bumps strictly centered around hair follicles. These are the primary source of the Staphylococcus aureus colonization.
Crusting and Erosions: As pustules rupture, they form thick, yellowish “honey-colored” crusts. If these are removed, they often leave behind raw, weeping erosions on the scalp.
Hemorrhagic Exudate: Bleeding may occur from the follicles with minimal friction, indicating deep-seated dermal inflammation.
The End-State: Cicatricial Scarring
The goal of any Folliculitis Decalvans treatment is to prevent the disease from reaching this final, irreversible stage:
Follicular Loss: The scalp loses its natural “pores” or follicular openings.
Scar Tissue (Fibrosis): The skin becomes smooth, shiny, and ivory-white. This is the biological “dead end” where the hair bulge stem cells have been entirely replaced by collagen.
Patchy Alopecia: Unlike the diffuse thinning seen in hormonal hair loss, this appears as distinct, expanding “islands” of baldness that eventually merge.
4: Diagnosis & Differential Diagnosis
A precise diagnosis is the cornerstone of any effective Folliculitis Decalvans treatment plan. Because FD can mimic other scalp conditions, clinicians must rely on high-magnification imaging and histopathology to confirm the presence of neutrophilic scarring.
Dermatoscopy Findings (Trichoscopy)
Trichoscopy allows for a non-invasive look at the active borders of the disease. In a clinical setting, the following findings are diagnostic hallmarks of FD:
Perifollicular Erythema: Intense redness and inflammation concentrated specifically around the hair shafts.
Yellowish Scales and Crusts: Accumulation of inflammatory exudate and keratin at the follicular base.
Loss of Follicular Openings: The absence of “pores” in the center of the patch, indicating that scarring has already begun.
Targeted Hair Tufts: Observing “doll-like” tufts (multiple hairs from one opening) under magnification.
Biopsy Protocols: The 4mm Punch
While clinical signs are often strong, a skin biopsy remains the gold standard for a definitive diagnosis.
The 4mm Punch Biopsy: A small tissue sample is taken from the active leading edge of a lesion to capture the neutrophilic inflammation in progress.
Histopathology: The lab looks for a dense infiltration of neutrophils around the upper part of the hair follicle and the presence of intrafollicular bacteria.
Vertical and Horizontal Sectioning: This helps the pathologist see the destruction of the hair bulge and the replacement of the follicle with fibrous tissue.
Distinguishing from Scalp Acne and Mimickers
It is easy to misdiagnose FD as a standard infection or “scalp acne.” However, the management of these conditions is vastly different.
| Feature | Folliculitis Decalvans | Standard Scalp Acne | Folliculitis Keloidalis Nuchae (FKN) |
| Scarring | Yes (Permanent) | No (Temporary) | Yes (Keloid-like) |
| Primary Site | Vertex/Crown | Diffuse | Nape of the neck/Occiput |
| Hallmark | Tufted Hairs | Comedones/Pimples | Thick, itchy bumps/keloids |
Clinical Note: While our guide on Glycolic Acid for Scalp Acne (Article #120) is excellent for detoxing standard clogged pores, FD requires systemic medical intervention. Standard “detox” methods are insufficient to stop the neutrophilic destruction of the hair bulge stem cells.
2026 Evidence-Based Treatment Protocols
In 2026, the clinical landscape for Folliculitis Decalvans treatment has shifted toward aggressive, multi-modal strategies. The primary goal of medical intervention is to achieve rapid remission to “rescue” remaining hair follicles from irreversible scarring.
First-Line Antibiotics: The Gold Standard Combination
For active, pustular phases of the disease, combination antibiotic therapy is used to disrupt the S. aureus biofilm and reduce the bacterial load.
Clindamycin and Rifampicin: This combination (typically 300 mg of each twice daily) remains a cornerstone of treatment. Rifampicin’s ability to penetrate biofilms, paired with Clindamycin’s anti-staphylococcal properties, often induces significant clinical improvement.
Treatment Duration: Most protocols suggest a 10 to 12-week course to ensure deep-seated inflammation is fully suppressed.
Anti-Inflammatory Agents
Since FD is driven by an overactive neutrophilic response, suppressing the immune system is a critical component of a Folliculitis Decalvans treatment plan.
Corticosteroids: Topical high-potency steroids or intralesional injections (Triamcinolone acetonide) are used to quickly calm localized flares and reduce scalp pain.
Dapsone: Used for its specific anti-neutrophilic properties, Dapsone can be an effective long-term maintenance option for patients who do not respond to traditional antibiotics.
Modern Advancements & 2026 Breakthroughs
As our understanding of molecular pathways grows, newer “off-label” treatments are becoming more common in clinical practice.
Biologics (TNF-alpha Inhibitors): For refractory (stubborn) cases, biologics like Adalimumab or Infliximab are showing promise by blocking the systemic inflammatory cytokines that fuel the scalp destruction.
Adjuvant Therapy (LLLT): Low-Level Laser Therapy (also known as Red Light Therapy) is increasingly utilized as a supportive tool. As discussed in Article #121 (Red Light Therapy for Hair Growth), these wavelengths can modulate cellular activity and reduce the overall inflammatory markers in the scalp tissue.
Isotretinoin: The Role in Long-Term Remission
Oral Isotretinoin is often utilized when traditional antibiotics fail to sustain remission.
Why It Works: It significantly reduces sebum production (which bacteria feed on) and alters the follicular environment, making it less hospitable to Staphylococcus aureus.
When to Use It: It is typically reserved for the “maintenance” phase or for patients with co-existing severe scalp acne to prevent further pustule formation.
Expert Note: Any Folliculitis Decalvans treatment must be monitored by a specialist, as long-term use of these medications requires regular blood work to monitor liver and kidney function.
6: Clinical Scalp Care & Maintenance
Beyond systemic medication, the success of a Folliculitis Decalvans treatment plan depends heavily on daily scalp hygiene. Because the scalp’s environment is compromised, maintenance must focus on reducing bacterial load without further damaging the biological recovery phases of the skin.
Antiseptic Washes & Barrier Protection
Managing the microbial landscape of the scalp requires specific antiseptic agents.
Medical-Grade Washes: Clinicians often recommend Hibiclens (Chlorhexidine) or 2% Pyrithione Zinc washes to target the S. aureus colonization directly.

Expert Recommended
Hibiclens Antiseptic Skin Cleanser
Target deep-seated Staphylococcus aureus colonization and disrupt the “vicious cycle” of inflammation effectively.
Protecting the Acid Mantle: It is vital to use these treatments carefully to avoid disrupting the skin barrier.
Balanced Care Strategy: It is vital to preserve the scalp’s moisture levels to mitigate secondary irritation while simultaneously targeting the primary infection. Maintaining this equilibrium is a core principle of biological recovery, as detailed in our comprehensive guide on Healing the Skin Barrier .

Medical-Grade Scalp Recovery Serum
Clinically formulated to support the skin barrier during biological recovery.
Biofilm Management: Why Standard Shampoos Fail
A common reason for treatment resistance is the formation of a biofilm—a protective “shield” created by bacteria.
Standard Shampoos: Most commercial shampoos only clean the surface and cannot penetrate the dense biofilm matrix.
Medical-Grade Cleansers: Clinical cleansers are formulated with surfactants and active ingredients designed to break down these microbial layers.
Persistence: Consistent use of targeted cleansers is necessary to prevent the bacteria from rebuilding their defenses within the hair follicles.
Avoiding Triggers
Managing FD also requires lifestyle adjustments to reduce physical and environmental stressors on the hair follicles:
Heat: Avoid high-temperature styling tools and very hot showers, as heat can exacerbate inflammatory flushing and pruritus.
Friction: Minimize tight hats, aggressive towel-drying, or frequent scratching, which can rupture pustules and spread the infection.
Occlusive Products: Steer clear of heavy waxes, oils, or thick styling creams. These “occlusive” products can trap bacteria and sebum, creating an anaerobic environment that fuels the “vicious cycle” of neutrophilic inflammation.
7: Prognosis – Can Hair Grow Back?
One of the most difficult conversations in a Folliculitis Decalvans treatment plan involves setting realistic expectations for hair recovery. Because this is a primary scarring alopecia, the biological outcome differs significantly from common thinning or shedding.
The Reality Check: The Permanent Nature of Scarring
The biological reality of FD is that once the hair follicle has been replaced by fibrous scar tissue, hair cannot grow back.
Destruction of the Bulge: As discussed in the pathophysiology section, the inflammation destroys the stem cells in the hair bulge.
Fibrosis: When these stem cells are gone, the body “repairs” the site with a collagen-dense scar rather than regenerating a new hair follicle.
Irreversibility: No serum, vitamin, or medication—including the ones mentioned in our guide on Best Scalp Serums (Article #31)—can revive a follicle that has reached this end-state of cicatricial fibrosis.
Goal of Therapy: Shifting the Focus
For many patients, the initial hope is for total regrowth. However, the primary clinical objectives of any effective Folliculitis Decalvans treatment must pivot toward:
Arresting the Spread: The most critical goal is to stop the inflammatory border from expanding and destroying the remaining healthy follicles.
Symptom Management: Eliminating pain, burning, and the social distress caused by active pustules and crusting.
Long-Term Remission: Maintaining a stable, non-inflammatory state for years to prevent future flare-ups.
Surgical Options: Hair Transplants
For those with stable, inactive scarring, a hair transplant might seem like a solution, but it requires extreme caution and strict clinical timing.
The 2-Year Rule: Most specialists will only consider surgical intervention after at least 2 years of proven, complete clinical remission without any medication.
Risk of Reactivation: Performing surgery on a scalp where the immune system is still “primed” for neutrophilic attack can cause the disease to reactivate, leading to the failure of the new grafts.
Scalp Health First: Ensuring the surrounding skin barrier is healthy and free of Staphylococcus aureus colonization is a prerequisite for any successful surgical outcome.
8: Conclusion – The Path Forward for Scalp Health
The management of Folliculitis Decalvans is a clinical marathon, not a sprint. The biological window for saving hair follicles is narrow, making the importance of early intervention the single most critical factor in your prognosis. By identifying symptoms before they transition into the “End-State” of cicatricial fibrosis, you can successfully arrest the spread and preserve your existing hair density.
At Nagash Health, our philosophy centers on the integration of clinical medicine and holistic scalp wellness. While systemic antibiotics and anti-inflammatory protocols are necessary to stop neutrophilic destruction, maintaining the scalp’s skin barrier and managing the microbial environment are what sustain long-term remission. True scalp health is achieved when we bridge the gap between aggressive medical intervention and evidence-based daily care.
Frequently Asked Questions (FAQ)
Is Folliculitis Decalvans contagious? No. While Staphylococcus aureus is involved, the condition is driven by an abnormal host immune response, not a simple infection that can be passed to others.
Can I use Minoxidil for Folliculitis Decalvans? Minoxidil should only be used in stable, non-inflammatory areas. Using it on active pustules can cause severe irritation and may worsen localized inflammation.
How long does it take to see results from Folliculitis Decalvans treatment? Clinical improvement in pain and pustule reduction is often seen within 4 to 8 weeks, but a full course of combination therapy usually lasts 10 to 12 weeks to ensure deep-seated remission.
Will red light therapy help my hair grow back? Red light therapy (LLLT) is an adjuvant tool to reduce inflammation. It can help “rescue” follicles currently under attack, but it cannot regrow hair in areas where the skin has already scarred over.
Medical Disclaimer
The information provided by Nagash Health is for educational and research purposes only. Folliculitis Decalvans is a complex medical condition that requires a diagnosis from a board-certified dermatologist. Always seek the advice of a physician before starting any new medication or treatment protocol.